Asthma
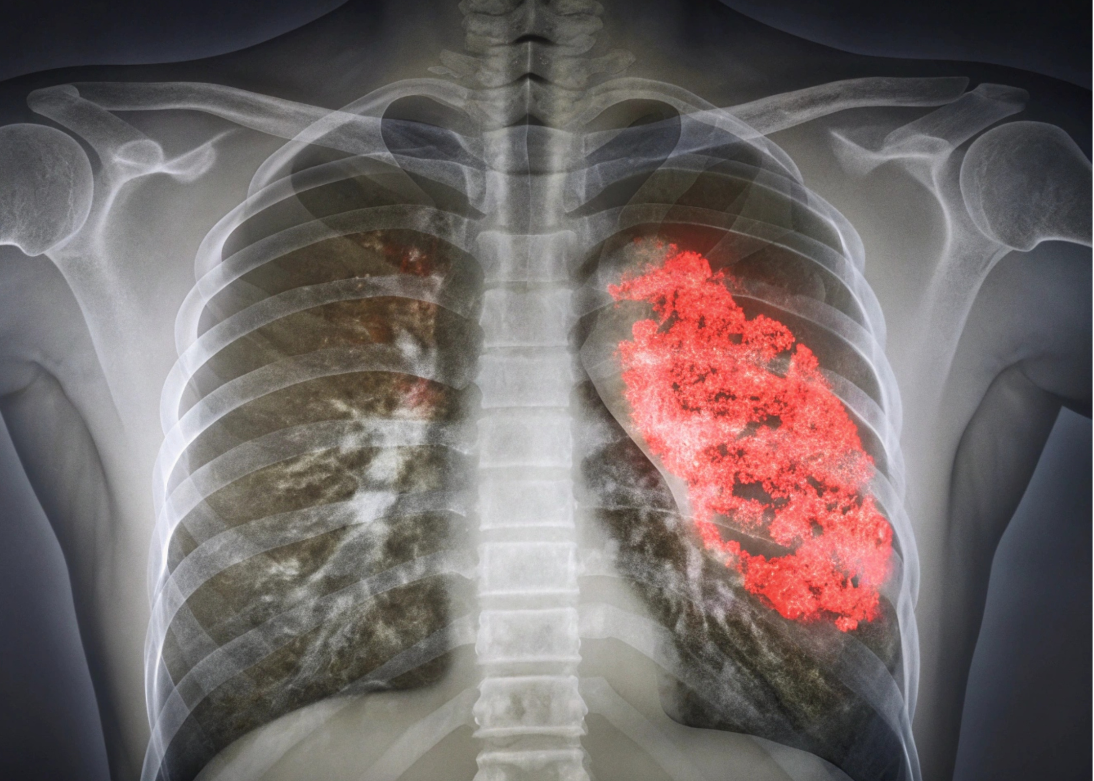
Asthma is a chronic condition in which your airways narrow, swell, and may produce extra mucus. This makes breathing difficult and can trigger coughing, wheezing, and episodes of shortness of breath. Symptoms can range from occasional discomfort to severe, life-threatening attacks.
Although asthma cannot be cured, it can be controlled. Because asthma often changes over time, it is important to work closely with your doctor to track symptoms and adjust treatment as needed.
Symptoms
Asthma symptoms vary from person to person. You may experience infrequent attacks, symptoms only during certain activities (such as exercise), or persistent daily symptoms.
- Shortness of breath
- Chest tightness or pain
- Wheezing when exhaling (common in children)
- Trouble sleeping due to coughing, wheezing, or breathlessness
- Coughing or wheezing triggered by respiratory infections like cold or flu
Signs your asthma may be worsening
- More frequent or bothersome symptoms
- Increasing difficulty breathing, as shown on a peak-flow meter
- Needing a quick-relief inhaler more often
Common triggers
- Exercise in cold, dry air
- Workplace irritants (chemical fumes, gases, dust)
- Airborne allergens such as pollen, mold spores, cockroach particles, and pet dander
Treatment Options
Managing asthma usually involves a combination of lifestyle adjustments and medications tailored to your needs. Your healthcare provider may recommend one or more of the following therapies:
- Bronchodilators: Relax airway muscles, making breathing easier and helping mucus move out. Used for quick relief in both intermittent and chronic asthma.
- Anti-inflammatory medicines: Reduce airway swelling and mucus production. Taken daily to control chronic symptoms.
- Biologic therapies: Advanced injections or infusions for severe asthma when other medicines are not enough.
- Delivery methods: Metered-dose inhalers, nebulizers, dry-powder inhalers, or oral medications—chosen based on symptom severity and patient preference.
Some patients may also need medications to control allergy-related congestion. Always consult your pulmonologist before starting decongestants, corticosteroid nasal sprays, leukotriene inhibitors, or immunotherapy.
Stick to your asthma action plan, schedule regular reviews, and notify your doctor if you notice changes in symptoms or inhaler use.





.png)
.png)

.png)
